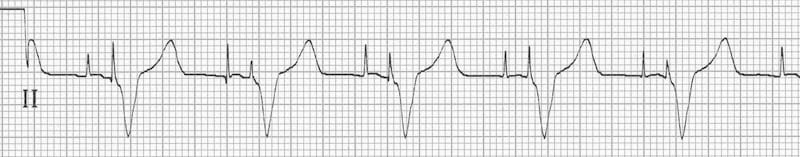
Several days later, the patient, the patient had a cardiac resynchronization device inserted by the Electrophysiology team and she was subsequently transferred out of the ICU 8 days after her initial admission in stable condition. Shortly thereafter, we replaced the transvenous pacemaker from her left internal jugular vein with a transvenous pacemaker from the left femoral vein to facilitate the insertion of a permanent pacemaker. With this VDI pacing instituted, the patient’s cardiac indices improved significantly and she was able to be weaned off all of her inotropes and vasopressors (see Fig. 2A–F) with the goal of increasing stroke volume due to re-establishing consistent atrial contribution to ventricular filling (atrial kick). This allowed for sensing of atrial activity (p-waves) and thus permitted atrio-ventricular (AV) synchronized pacing (see Fig. 
In an effort to further augment the patient’s cardiac output on POD 4, we attached a stiff temporary pacemaker wire to a standard orogastric (OG) tube and inserted it into the patient’s mid-esophagus. 1C) of note, the patient was on similar doses of vasopressors and inotropes at this juncture. Despite pacing at a higher rate than the patient’s intrinsic ventricular escape rate, the patient’s cardiac indices remained poor (see Fig. We subsequently inserted a transvenous right ventricular pacemaker wire as the epicardial temporary wires inserted at the time of surgery were inconsistently capturing despite increased output settings. Without mechanical support, the patient’s hemodynamic status remained tenuous and she still required pacing as her underlying heart rate was in the 40 s (see Fig. With her underlying hypoxemia and the new evidence of a PFO, we removed the patient’s IABP in an attempt to improve the right atrium to left atrium pressure gradient leading to interatrial shunting. To further aid with her hemodynamic status and manage her acidosis, she was started on inhaled nitric oxide (iNO) as well as continuous renal replacement therapy (CRRT). Prosthetic and native valve function were normal. A transthoracic echocardiogram post-operatively displayed a left ventricular ejection fraction of 31% with a severely impaired right ventricle and a patent foramen ovale (PFO) with a right-to-left shunt. On postoperative day (POD) one, cardiogenic shock persisted and the patient demonstrated significant hypoxemia. Her total time on cardiopulmonary bypass was 321 min and her aortic cross-clamp time was 277 min. Furthermore, she was pacer-dependent for complete heart block and was being paced via epicardial leads (VVI). She also required norepinephrine 0.5 μg/kg/min, epinephrine 0.5 μg/kg/min, vasopressin 2 units/hour, and milrinone 0.50 μg/kg/min infusions to support her blood pressure and cardiac output (see Fig. She was admitted to the cardiac surgery intensive care unit (ICU) post-operatively and required mechanical support with an intra-aortic balloon pump (IABP). She was put back on bypass and air was removed from her right coronary artery at this juncture, a transesophageal echocardiogram showed grossly normal left ventricular functional with reduced right ventricular function. 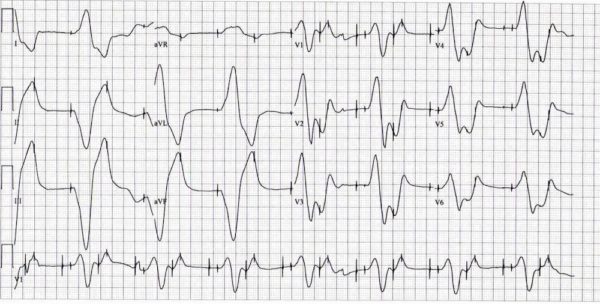 
She had a complicated intra-operative course whereby she decompensated after she was taken off cardiopulmonary bypass and her chest was closed. Of note, the patient needs to have underlying organized atrial activity for this setup to work.Ī 63-year-old female with heart failure, coronary artery disease, mitral regurgitation, bicuspid aortic valve, and a left atrial (LA) myxoma underwent coronary artery bypass grafting surgery in addition to the myxoma resection, mechanical aortic and mitral valve replacements. In hemodynamically unstable post-cardiac surgery patients with complete heart block in whom VVI pacing fails to improve their clinical status, clinicians should consider VDI pacing with an orogastric atrial sensing pacemaker lead, in consultation with the cardiac surgeon and the electrophysiology team. This was done temporarily to stabilize the patient’s hemodynamic status while awaiting a permanent pacemaker implantation. We describe a novel technique of attaching a temporary pacemaker wire to an orogastric tube to sense atrial p-waves and pace the ventricle transvenously to perform AV sequential pacing. With VVI pacing proving ineffective, it was postulated that the patient may benefit hemodynamically from AV sequential pacing, re-establishing her atrial kick. Our case highlights the management of a 62-year-old female with cardiogenic shock post-cardiac surgery with concomitant complete heart block. Post-operative atrio-ventricular (AV) block after cardiac surgery is not uncommon in high-risk patients.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
